Abstract
Background
Evidence supports the role of rehabilitation in the management of lung cancer symptoms. Previous research reports that rehabilitation needs are inadequately recognised and managed, which may adversely affect patients’ quality-of-life and create burden for caregivers.
Aims
This study aims to explore the perceptions of palliative care and respiratory multidisciplinary team (MDT) members about the role of rehabilitation for lung cancer patients, examine patterns of referral for lung cancer patients to rehabilitation services, and highlight the barriers which prevent the referral of lung cancer patients to rehabilitation services.
Methods
Questionnaires were completed by MDT members within a regional cancer network during June 2010.
Results
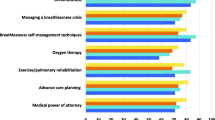
Fifty-nine healthcare professionals participated. Ninety-four per cent of respondents perceived their patients had rehabilitation needs. Referral most commonly occurred during the palliative (29.6 %) and post-treatment (23.7 %) disease phases. Barriers to referral included “lack of knowledge of services or referral mechanisms” (28.8 %), “waiting lists” (28.8 %) and the perception that patients “do not desire rehabilitation” (22 %). Rehabilitation needs were most frequently discussed at palliative in-patient MDT meetings [reported as “often” by 37 (62.7 %) respondents] and least discussed at lung MDTs (half of respondents reporting that rehabilitation was “never” discussed). Rehabilitation services were considered adequate by 39 % of respondents.
Conclusions
Long waiting times and lack of knowledge of services are among several factors that may prevent lung cancer patients being offered rehabilitation. In order to improve the quality of care delivered to cancer patients, it is important to remove barriers that affect delivery of rehabilitation services.



Similar content being viewed by others
References
Cancer Research UK. Lung cancer—UK incidence statistics. http://info.cancerresearchuk.org/cancerstats/types/lung/incidence/#source1 (accessed on January 2012)
Jemal A, Bray F, Center MM et al (2011) Global cancer statistics. CA Cancer J Clin 61:69–90
Sanders SL, Bantum EO, Owen JE et al (2010) Supportive care needs in patients with lung cancer. Psychooncology 19:480–489
Temel JS, Greer JA, Muzikansky A et al (2010) Early palliative care for patients with metastatic non-small-cell lung cancer. N Engl J Med 363:733–742
Riesenberg H, Lubbe AS (2010) In-patient rehabilitation of lung cancer patients—a prospective study. Support Care Cancer 18:877–882
Ross L, Petersen MA, Johnsen AT, Lundstrom LH, Groenvold M (2011) Are different groups of cancer patients offered rehabilitation to the same extent? A report from the population-based study “The Cancer Patient’s World”. Support Care Cancer. doi: 10.1007/s00520-011-1189-6
Rankin J (2008) Rehabilitation in cancer care. Wiley-Blackwell, Oxford
National Institute for Clinical Excellence (2004) Guidance on cancer services: improving supportive and palliative care for adults with cancer
Bredin M, Corner J, Krishnasamy M, Plant H, Bailey C, A’Hern R (1999) Multicentre randomised controlled trial of nursing intervention for breathlessness in patients with lung cancer. BMJ 318:901–904
Corner J, Wright D, Hopkinson J, Gunaratnam Y, McDonald JW, Foster C (2007) The research priorities of patients attending UK cancer treatment centres: findings from a modified nominal group study. Br J Cancer 96:875–881
Bausewein C, Booth S, Gysels M, Higginson I (2008) Non-pharmacological interventions for breathlessness in advanced stages of malignant and non-malignant diseases. Cochrane Database Syst Rev 2:CD005623
Hately J, Laurence V, Scott A, Baker R, Thomas P (2003) Breathlessness clinics within specialist palliative care settings can improve the quality of life and functional capacity of patients with lung cancer. Palliat Med 17:410–417
Andersen C, Adamsen L, Moeller T, Midtgaard J, Quist M, Tveteraas A, Rorth M (2006) The effect of a multidimensional exercise programme on symptoms and side-effects in cancer patients undergoing chemotherapy–the use of semi-structured diaries. Eur J Oncol Nurs 10:247–262
Luebbert K, Dahme B, Hasenbring M (2001) The effectiveness of relaxation training in reducing treatment-related symptoms and improving emotional adjustment in acute non-surgical cancer treatment: a meta-analytical review. Psychooncology 10:490–502
Wilkinson S, Barnes K, Storey L (2008) Massage for symptom relief in patients with cancer: systematic review. J Adv Nurs 63:430–439
Dimeo F, Rumberger BG, Keul J (1998) Aerobic exercise as therapy for cancer fatigue. Med Sci Sports Exerc 30:475–478
Dimeo F, Schwartz S, Wesel N, Voigt A, Thiel E (2008) Effects of an endurance and resistance exercise program on persistent cancer-related fatigue after treatment. Ann Oncol 19:1495–1499
Cramp F, Daniel J (2008) Exercise for the management of cancer-related fatigue in adults. Cochrane Database Syst Rev 2:CD006145
Fox SW, Lyon DE (2006) Symptom clusters and quality of life in survivors of lung cancer. Oncol Nurs Forum 33:931–936
Currow DC, Abernethy AP (2011) Therapeutic nihilism: the next hurdle in improving the treatment of breathlessness. Curr Opin Support Palliat Care 5:69–70
NHS National Cancer Action Team (2009) Rehabilitation care pathway: lung. Crown Copyright
Cheville AL, Beck LA, Petersen TL, Marks RS, Gamble GL (2009) The detection and treatment of cancer-related functional problems in an outpatient setting. Support Care Cancer 17:61–67
National Institute for Clinical Excellence (2002) Principles for best practice in clinical audit. Radcliffe, Oxford
Lynch J, Goodhart F, Saunders Y, O’Connor SJ (2010) Screening for psychological distress in patients with lung cancer: results of a clinical audit evaluating the use of the patient Distress Thermometer. Support Care Cancer 19:193–202
Cooley ME, Short TH, Moriarty HJ (2003) Symptom prevalence, distress, and change over time in adults receiving treatment for lung cancer. Psychooncology 12:694–708
Lowe SS (2011) Physical activity and palliative cancer care. Recent Results Cancer Res 186:349–365
Maddocks M, Mockett S, Wilcock A (2009) Is exercise an acceptable and practical therapy for people with or cured of cancer? A systematic review. Cancer Treat Rev 35:383–390
Maddocks M, Armstrong S, Wilcock A (2011) Exercise as a supportive therapy in incurable cancer: exploring patient preferences. Psychooncology 20:173–178
Lowe SS, Watanabe SM, Baracos VE, Courneya KS (2010) Physical activity interests and preferences in palliative cancer patients. Support Care Cancer 18:1469–1475
Temel JS, Greer JA, Goldberg S, Vogel PD, Sullivan M, Pirl WF et al (2009) A structured exercise program for patients with advanced non-small cell lung cancer. J Thorac Oncol 4:595–601
NHS National Cancer Action Team. Holistic needs assessment for people with cancer. http://www.ncsi.org.uk/wp-content/uploads/Holistic-Needs-Assessment-practical-guide.pdf (accessed January 2012)
Wade DT (2001) Research into rehabilitation. What is the priority? Clin Rehabil 15:229–232
Wade DT (1998) Evidence relating to goal planning in rehabilitation. Clin Rehabil 12:273–275
Korner M (2010) Interprofessional teamwork in medical rehabilitation: a comparison of multidisciplinary and interdisciplinary team approach. Clin Rehabil 24:745–755
Funding
This research received no specific grant from any funding agency in the public, commercial, or not-for-profit sectors.
Competing interest
None declared.
Ethics
This study did not require ethical approval as it has been classified as an audit by the Research and Development department of Marie Curie Palliative Care Institute Liverpool, University of Liverpool (MCPCIL).
Author information
Authors and Affiliations
Corresponding author
Rights and permissions
About this article
Cite this article
Nwosu, A.C., Bayly, J.L., Gaunt, K.E. et al. Lung cancer and rehabilitation—what are the barriers? Results of a questionnaire survey and the development of regional lung cancer rehabilitation standards and guidelines. Support Care Cancer 20, 3247–3254 (2012). https://doi.org/10.1007/s00520-012-1472-1
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s00520-012-1472-1